A variety of drugs and drug combinations carry the risk of fatal overdose. If you suspect someone is experiencing an overdose it is critical to call 911.
However, in the case of an opioid overdose, which can be caused by heroin and prescription pain medications like Vicodin, OxyContin and Percocet, using naloxone (also known by the brand name Narcan) can potentially save someone’s life — even before first responders arrive.
Naloxone is an opioid overdose reversal medication, available either as a nasal spray or an injector. An opioid overdose occurs when opioids have fully blocked the brain’s opioid receptors, causing a person’s breathing to slow down and ultimately stop. Naloxone works by knocking the opioids out of the receptors in the brain where they are having their effect and preventing them from returning. When enough naloxone is administered, breathing will return to normal, saving an individual from the brink of death.
Anyone can carry naloxone for any reason. No doctor’s prescription is required to purchase naloxone from a pharmacy. A few reasons you may consider carrying naloxone include:
Anyone using opioids, whether for recreational purposes or otherwise, can be at risk for overdose. Having naloxone readily available does not encourage risky drug use but it does mean someone who is experiencing an overdose has a better chance of surviving and eventually getting the help they need.
It is important to note that higher doses of naloxone are becoming more common for some opioids, especially fentanyl. However, research has shown that more naloxone can also cause severe withdrawal symptoms, which can have serious and even life-threatening health effects, and that it is not necessarily beneficial to administer more.
An overdose can occur anywhere from 20 minutes to two full hours after use of substances. Signs of an overdose include:
If you suspect an overdose and your child is unresponsive, call 911. To check if your loved one is unresponsive, first, try getting their attention by calling their name or saying phrases that might alarm them, such as “I’m going to call the police.” If that doesn’t elicit a response, then try rubbing their chest firmly with your knuckles to wake them.
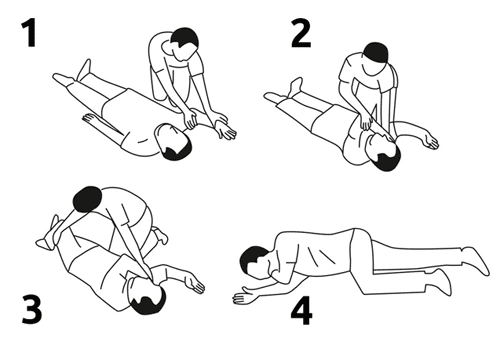
If they remain unresponsive, and you must leave them alone to make the call, it’s important to put them in the recovery position — on their side with legs bent and head resting on the arm on the floor (see image below). This is to avoid aspiration if they vomit. Give the address or location and as much information as you can (e.g., unconscious, not breathing, drugs used if known, etc.).
Naloxone is only effective in the case of an opioid overdose. However, if you are unsure of the substance(s) involved, it’s best to err on the side of caution and administer it. Naloxone is not known to cause any harm in the case of a non-opioid overdose.
If they have labored breathing or are not breathing at all, it is vital to conduct rescue breathing. Tilt the head back, pinch the nose closed and give one slow breath every 5 seconds until they resume breathing on their own or until the paramedics arrive. Watch to see that their chest rises and falls with each breath.
Once they are breathing on their own, place them in the recovery position until paramedics arrive. Comfort them as they may be confused, upset and going through withdrawal (feeling sick from a lack of opioids if their body is dependent on them) when revived. Do not allow them to use drugs.
Once your loved one has been stabilized, this may be an opportunity to suggest detox and treatment.

Learn more about how you can respond to an overdose