 Doctors at Stanford University are trying to help people dependent on opioid painkillers break the vicious cycle in which physical pain and emotional distress exacerbate one another.
Doctors at Stanford University are trying to help people dependent on opioid painkillers break the vicious cycle in which physical pain and emotional distress exacerbate one another.
Through an intensive week-long inpatient program that combines physical and occupational therapy, lifestyle and behavioral modifications and medication, patients have experienced significant improvements in pain levels, emotional functioning and physical activity, according to Ravi Prasad, PhD, Assistant Chief of Stanford’s Division of Pain Medicine.
Dr. Prasad will be speaking about the program and its results at the upcoming American Psychological Association meeting in Toronto.
People in chronic pain can become dependent on painkillers because they believe the pills can cure their pain, Dr. Prasad explained. “But pain pills aren’t a magic bullet, so they have an emotional setback when they try it and it doesn’t fix the problem,” he says.
The Stanford program takes a different approach, by using a combination of medical, physical and behavioral management to help patients learn to cope with their pain. “They learn to treat it like other chronic conditions, such as diabetes and asthma,” he says. “The goal is to improve the quality of life and functioning.”
The first thing the Stanford doctors do is to look at all aspects of a patient’s medical condition to make sure their chronic pain is not being caused by a treatable condition. “We see if the person can be helped by injection therapy, pain pump, spinal cord stimulators, or surgery,” he says. “We see if they are on the most appropriate medication at the most appropriate level.”
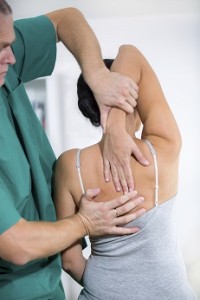
The next step is to examine the patient’s physical conditioning. “With chronic pain, there is a natural tendency to guard the part of the body that is hurting,” Dr. Prasad notes. “If the lower back hurts, you’ll try to protect it. But minimizing use of that part of the body can start to cause atrophy of muscles that you’re trying to protect. This can worsen the condition and cause you to overuse other parts of the body to compensate.” Patients work with a physical therapist or rehabilitation specialist to correctly learn how to use the part of the body that is hurting.
The third step is teaching the patient lifestyle modification to deal with their chronic pain. “Pain can affect all areas of a person’s life,” Dr. Prasad says. “Your activity levels decrease, and you can experience depression, anger, anxiety and sleep disturbances. For many of our patients, pain is the focus of their life. We help them learn to decentralize the role of pain in their life.”
Patients learn how stress influences their pain. Stress activates the sympathetic nervous system, which in turn can exacerbate underlying pain. Emotional responses to pain—including anxiety, guilt, anger, and sadness—all feed into this cycle resulting in a physically and emotionally overwhelming situation that can feel inescapable.
The program teaches patients breathing and relaxation exercises, activity regulation, and cognitive restructuring, all of which is geared toward breaking the pain cycle. Using these skills, patients learn how to approach a day when they wake up with a high level of pain. “If you think, ‘This will never end, life is terrible, the whole day is ruined,’ that will directly influence your behaviors, emotions, and physical state.” Dr. Prasad observed. “The body’s stress response will kick in and increase pain.”
Patients are taught to stop and ask themselves if these thoughts are helpful or accurate. “Ask yourself, ‘Is it true there’s nothing I can do to help the pain?’ You may not be able to fix the pain, but you can do things like breathing exercises to influence it. Is the day really ruined? Maybe once you’re up and moving, you can get something done. Think, ‘I’ll pace myself. This is just a flare, and the moment will pass. The day is not set yet.’” Such modification of thoughts can be a challenging process but it is one that can yield significant improvements in physical and emotional functioning.
Stanford’s inpatient program for chronic pain patients dependent on opioids lasts seven to 10 days. Most come in on very high doses of opioid medications and have a very low ability to function.
The patients are given painkillers in a dosage-blinded liquid form, so they don’t know how much of the actual medicine they are getting. They take the same volume of liquid every day, but the doctors manipulate the dosage. “We may increase the dose if a person is struggling to function and see if it shifts their activity pattern,” Dr. Prasad says. “If we see no change, then we can say their problems with functioning are not related to their dosage.”
It is not designed to be a detox program. “We are trying to optimize their medication,” Dr. Prasad says. “If we find there is an optimal dose we try to maintain it. We find in most cases, we are able to help people come completely off their medications or reduce their dosing by 75 percent. As we lower the dose, their functioning tends to improve.”
Patients have daily physical and occupational therapy sessions, as well as psychological therapy sessions. A study of 44 patients in the program found after seven to 10 days, they had significant decreases in scores on pain and depression. Most aspects of their mood improved, except for anger and hostility.
“Our goal is to help patients realize there is much more they can do to influence how they experience pain,” Dr. Prasad said. “You can’t will your pain away, but you can have much more power to influence it than you think. It’s not an all-or-nothing proposition.”
Published
July 2015
 Get Support
Get Support
